Last Updated on July 7, 2024 by Max
Introduction
Before discussing my personal journey with prostatitis and its management, it’s crucial to understand the theoretical backdrop that forms the basis of this approach. This will enable my readers to comprehend why this method differs from conventional ones and deserves some consideration.
Over the past six months, I’ve managed to alleviate all signs of prostatitis without stepping into a doctor’s office. The exact pathophysiology of prostatitis remains elusive. Hence, current medical interventions primarily aim to mitigate the associated symptoms. The prostate gland enlarges progressively through a man’s life, leading to Benign Prostatic Hyperplasia (BPH)—the most prevalent benign neoplasm in men. Approximately 50% of men aged 50-60 and 90% above 85 experience BPH. However, prostate enlargement does not necessarily correlate with symptom severity—this is subjective to each individual. Consequently, symptom severity is often the sole gauge of disease progression.
Considering this, my proposed strategy also emphasizes symptom alleviation rather than claiming to ‘cure’ the disease. Let’s first clarify some essential terminologies to preclude any misunderstandings.
Understanding the Prostate Gland
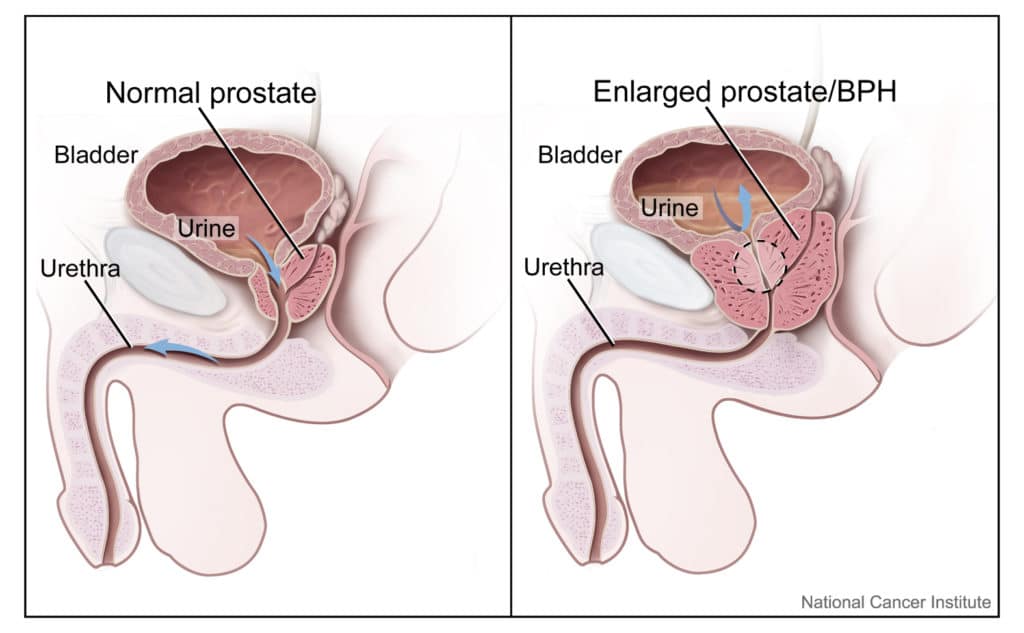
The prostate gland, a part of the male reproductive system in mammals, is a walnut-sized exocrine gland weighing around 11 grams (0.4 oz). Located beneath the bladder and positioned between the bladder and the penis, the urethral duct runs through the prostate tissue, conducting urine from the bladder through the penis. About 30% of semen constitutes prostate fluid, a milky alkaline mixture of enzymes, zinc, and simple sugars. This fluid protects, nourishes sperm, and assists in achieving fertilization.
Demystifying Prostatitis
Prostatitis, as defined by Wikipedia, is an inflammation of the prostate gland. The National Institute of Diabetes and Digestive and Kidney Diseases classifies prostatitis into four distinct forms: acute and chronic bacterial prostatitis, Chronic Pelvic Pain Syndrome (estimated to be 95% of prostatitis diagnoses), and asymptomatic inflammatory prostatitis. The first two forms are treated with antibiotics, while the third form is managed through various interventions such as medications, physical therapy, nerve modulators, phytotherapy, surgery, and more.
Prostatitis Symptoms
Prostate size can increase up to ten-fold with age. In about a third of men, this can compress the urethra, affecting urine flow, resulting in symptoms such as dribbling at the end, a difficult start, a thin stream, painful urination, pain in the pelvic area, and lower back pain, among other urogenital discomforts. It’s important to differentiate prostatitis from prostate cancer, as they share similar symptoms. However, prostatitis does not increase the risk of cancer. Thus, upon experiencing any signs of prostatitis, it’s essential to seek medical advice to determine the type of prostatitis and to evaluate the potential treatment options.
My Approach to Managing Prostatitis
When we delve deeper into the definition of prostatitis, inflammation emerges as a protective response against harmful stimuli such as pathogens, injured cells, or other irritants. It involves several defense mechanisms, including body temperature elevation, immune response, and molecular mediators designed to localize the affected site and restore tissue function.
Considering the prostate’s proximity to the bladder, urethra, and colon—bodily systems responsible for excreting liquid and fecal waste—it is continuously exposed to these irritants. Therefore, lifestyle habits, including diet, hydration, and smoking, play a significant role in triggering inflammatory processes in the prostate.
In this case, the primary objective should be to reduce the severity of symptoms by completely or partially resolving inflammation. Rather than delve into the pros and cons of other methods in this post, it’s worth noting that many have limited effectiveness and can cause numerous side effects, which can deter many.
Given these challenges, my primary focus was identifying herbs or natural substances with strong anti-inflammatory properties and minimal side effects and devising a method to effectively deliver these substances to the prostate.
Recipe for Prostate Inflammation Management
The following recipe proved to be highly effective for me, without any discernible side effects:
1. Shilajit; 150-200 mg
2. Eucalyptus leaves: 1 tablespoon
4. Water: 150-200 ml (5-6.7 oz)
Pour 150-200 ml of purified water into a glass mug, add one tablespoon of shredded Eucalyptus leaves, and boil for five minutes on low heat. Allow it to cool down to around 50 °C (122°F), strain to remove the debris, and then add 150-200 mg of Shilajit and stir until it dissolves.
Delivering the Anti-Inflammatory Decoction to the Prostate
Most anti-inflammatory tea recipes recommend consuming the tea twice a day for two or more weeks. However, considering the small size of the prostate gland, it’s questionable how much of the active substance can reach it after being ingested and digested. Not to mention the potential harm to the digestive system from regular consumption of biologically active tea, especially for those with existing digestive problems.
Considering these factors and the prostate’s proximity to the anus, I elected to deliver the anti-inflammatory decoction rectally.
Using the Rectum for Prostate Treatment
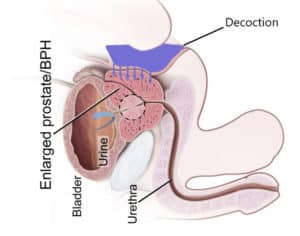
The rectum, the last few inches of the large intestine, directly adjoins the prostate. It plays a role in absorbing water and electrolytes from undigested food. Therefore, we can leverage this easily accessible location and the rectum’s absorption ability to effectively manage prostate inflammation.
Instructions for Using the Anti-Inflammatory Decoction
- Ensure your rectum is clean by using the toilet in the morning.
- The decoction should be warm but not scalding. Test by immersing your finger in it for five seconds. Use 150-200 ml (1.5-3 oz) of the prepared decoction per application.
- Lie on your stomach for one hour to allow the liquid to absorb from the rectum into the bloodstream and the surrounding organs.
- Repeat this procedure twice for one or two days. If you notice positive changes in your prostate, reduce the frequency to once a day for the next 7-10 days.
Despite the absence of prostatitis symptoms, remember that they can recur due to various factors. However, now you are well-equipped to manage it. Treat your prostate with the anti-inflammatory decoction 2-3 times at any sign of recurrence.
You may notice significant improvement after the second or third enema application, but this can vary. The warm temperature of the decoction relaxes the rectum and prostate, making them more receptive to the healing effects of the active ingredients in the liquid. Other herbs, such as Stinging Nettle leaves or roots and Green Tea, can also be used instead of Eucalyptus leaves.
Potential Outcomes of this Prostate Management Approach
- Total or partial reduction of prostatitis symptoms, often noticeable the day after treatment.
- Overall improvement of urogenital health and wellness in the pelvic region.
- Depending on your age, you might experience increased libido, stamina, and nocturnal erections as a side effect.
- Enhanced self-perception and confidence in life
Conclusion
In conclusion, I want to emphasize the importance of changing our attitudes toward prostate health. We often take for granted that our organs, such as the prostate, will continue to function without problems for years, just like our heart or other internal organs. However, this casual attitude can lead to neglect, resulting in prostatitis and associated symptoms. We need to learn how to care for our prostate, whether or not we have prostatitis.
The method I outlined above, describing how I managed my prostatitis, is simple and effective for alleviating inflammation in the prostate. It utilizes natural ingredients with potent anti-inflammatory properties and takes advantage of the rectal route to effectively deliver these substances to the prostate, leveraging the healing power of the decoction and the relaxing effect of its warmth.
In the next post, we will delve into why we’ve chosen these ingredients for the anti-inflammatory decoction, their specific properties, and any potential side effects.
Give it a Try!
While I found this approach to be effective for managing my prostatitis symptoms, remember that everyone’s body is unique, and what works for one person may not work for another. Always consult with your healthcare provider before starting any new treatment, especially if you have pre-existing health conditions or are currently on medications.
And remember, taking care of your overall health – eating a balanced diet, maintaining a healthy weight, exercising regularly, limiting alcohol intake, and avoiding smoking – can also contribute significantly to your prostate health. Prevention is always better than cure!






Hello, Makhsud, my X is passing through this very difficult time with prostate cancer, your site has brought me up to date information on the prostate grand.
This site would be very beneficial information for him. The only problem is that he is Latin Americano that has a limited understanding of the written English language.
What has captured my interest is your Holistic approach to the cure of the prostate because this is my approach also, not just in the prostate but with all our medical problems and would go as far as to say that if not some but all our problems radicate around Inflammation.
I concur with you in the use of ingredients with high Anti-inflammatory potions and also adds to my understanding that Mother Nature has the capacity to reverse all medical ailments. She has been with us from the beginning of man to the present date. The only difference is science has been able to prove her forth and there are some of the most extraordinary cures that are taking place in today’s world.
It is a very slow process and there are still too few doctors that follow that this protocol.
I believe that at some point in time this will be a norm in all households. This knowledge cannot be suppressed.
My approach is “There is always a better way as Mother Nature intended”. Thank you for your work in this field and bring about a better understanding of the Prostate gland.
Always a Better Way Linda
Dear Linda. Thank you so much for your supportive comment. I’m so sorry about your close man to have been diagnosed for prostate cancer. But I’m not surprised, unfortunately, I know that one in about 15 American in their 60s will be diagnosed for prostate cancer. This is a terrible statistics, but the statistics that should force every man to STOP and THINK.
I agree with you entirely; from the very start of any life, Mother Nature put the most powerful mechanism of self-healing. As a biologist, I know that even at the level of one cell we have hundreds of repair genes watching the correct work of our genetic material. Does it make sense to take so much care of a tiny cell and ignore such a complex organism as the human body?
Definitely, everybody has its intrinsic mechanism, I’d say, of correcting if something goes the wrong way. And we just have to learn how to help our body to do its work instead of suppressing the symptoms of illness with drugs.
Wishing you the best health
Makhsud
Hi Max
I have suffered an enlarged prostate and I could sense it was close to and pressing on my colon. Larry Clapp in his book mentions toxins that can transfer through the colon wall into the prostate. I have read about coffee enemas and as I was taking opioids for the pain I did some coffee enemas. They may have helped the liver but it seems they irritated the prostate. My urologist and any medical people I have spoken to discount my suggestions that constipation and toxins through the colon wall may cause problems. I have had an enlarged prostate to the point that the bladder was not fully emptying and the kidneys were unhappy so despite trying herbs etc I had to resort to a TURP procedure where my prostate was reduced in size ( 80cc to 34cc or is it grams).
Anyway all good now but I think I will follow your enema potion and diet suggestions. Thank you for imparting your knowledge and confirming the link between prostate issues and the colon toxins
Wayne
Hi Wayne
Thank you for your comment.
I’d like to draw your attention not as much to what I used to treat my prostate condition, as to the approach I used. There are hundreds of anti-inflammatory herbs and natural remedies that may be helpful for many but there is no one that could be a panacea for all. It is the same as we all are different and develop our illnesses differently. Any chronic illness develops in our body very slowly, sometimes for tens of years, changing the normal metabolism of the cells and organs for the sake of life-saving. All that means that if you got that condition you must be ready for the long fight to get back on track.
As to my personal experience, I found these four life-changing tricks very helpful:
1. Changing the diet to include more natural and organic foods and anti-inflammatory spices.
2. Avoid staying in the cold for a long time and sitting in the chair as well.
3. From time to time putting of enemas.
4. Stretching exercises for the pelvic area.
All this helps me to keep my prostate and all the other organs in that area happy and healthy.
More evidence-based information about the interconnection of prostate conditions and toxins and colon health you can find in some other posts:
https://yourhealthyprostate.com/prostate-cancer-looking-for-roots/
https://yourhealthyprostate.com/how-constipation-affects-your-prostate/
https://yourhealthyprostate.com/what-kind-of-meat-can-cause-prostate-cancer/
Hi Makhsud
Thanks for getting back to me.
I listened to a radio blog by Dr. Medici who said males don’t generally suffer testicular cancer because the testicles are always moving around etc.Interesting.
In this regard, I even considered prostate massage but found it too difficult to arrange.
But I am considering enemas not coffee as it seemed for me to cause some irritation. Are you able to suggest those herbs again you previously mentioned in your blog
In regard to your other suggestions, I went for a long run and jog on Saturday and it was cold although I was rugged up though there were times I felt the cold. Two days later, today, I have a headache and have sinus issues. So perhaps cold is an issue for the body.
At work, I did ask for a standing desk. I have changed my diet to more ketogenic. You have probably read the book by Larry Clapp. He has some good suggestions. But I am sure the constipation time wastes are held in the colon close to wall separating it from the prostate.
My wife recently died of gall bladder cancer. looking back I recall she never drank much water. I reckon dehydration may have contributed to or caused her cancer. In fact, dehydration may be a cause for all cancers. If the cells don’t get enough hydration they are unable to get rid of wastes. Cells are always dying and regenerating. I understand the cells in parts of the eyes regenerate in days. We are made up of 60-70% water so could it not be plausible that dehydration stops this natural process and may lead to cancer in a particular part of the body?
Cheers
Wayne
Hi Wayne
I wouldn’t say that “males don’t generally suffer testicular cancer.” Just googled out and found “Testicular cancer is the most frequently diagnosed form of cancer in men between the age of 15 to 44-years.” Yes, it is one of the most curable forms of cancer, but anyway. And the movements of the testicles has nothing to do with their vulnerability to cancer. To be precise, they are not moving more than any other part of the body.
Regarding the prostate massage, I do not think that it’s really difficult to arrange at home conditions, there are lots of prostate massagers on the market, but I’m not sure about their efficacy.
Unfortunately, the most potent anti-inflammatory remedies are spices such as turmeric, ginger, or coriander which may irritate the prostate as well. So you cannot use them with enemas but I’d recommend them to add to your everyday diet.
As to my suggestions in my blog, at least they worked for me. As I noted in the blog I excluded Willow Herb from my recipe, because of its strong hormonal effect. Willow Herb (as tea) is one of the most popular herbs recommended for prostate issues. It might need to set the effective healing concentrations of the herb in enema solution.
In regard to your running exercises, I am an opponent of long runnings, especially in cold. The best what I’d suggest is fast walking with wide steps for 30-60 min a day. And it shouldn’t be stressful for you.
I’d strongly suggest some stretching exercises, which I found very useful. (https://yourhealthyprostate.com/cure-prostatitis-and-chronic-pelvic-pain-syndrome-by-chinese-medicine-practices/). I’m doing stretching on the bench every day for about 20-30 min on each leg. You just forget heavy legs, lower back pain and it regulates circulation in the pelvic area best of all.
Yes, it’s hard not to agree with you about dehydration. And I hope you know that the tap water must be filtered.
Best regards
Makhsud
Hi! Have you tried supplements that include palmetto saw zinc and lycopene? I’ve read that they are of great help when it comes to dealing with prostatitis. I found this article about it: best-prostate-treatment-over-the-counter-in-2020.
Don’ t know if those are any good , tho!
Hi. Thank you for your question. Definitely, all the ingredients of the supplements are thought to be helpful in treating prostate symptoms. I tried some supplements presented in that post, ProstaGenix, for example, and a few saw palmetto extracts. Unfortunately, in the long run, none of them were helpful. What does modern science say about saw palmetto read here: https://yourhealthyprostate.com/does-saw-palmetto-work-in-treating-enlarged-prostate-symptoms/ and make your choice.
Have a great weekend!
Hello,
Are there any alternatives to using the rubber enema, maybe something I could drink to cleanse my colon, and if so, what is the procedure. I don’t think I will be able to use an enema 2 times a day, it may prove to be very difficult for me. Thank you!
Hi Gabriel
The procedure described in the post aims to deliver anti-inflammatory decoction into the prostate gland rather than the cleansing of the colon. We are not considering the whole large intestine, just only the last small part called the rectum which is in contact with the prostate. Depending on your body size the optimal tolerable amount of the decoction may range from 50 to 150 ml. It usually takes from 30 to 60 min for the whole decoction to absorb through the walls of the rectum without any bothering side effects.
But anyway, if you feel that enemas are not a good fit for you you can find some other alternative approaches to treat prostate issues here: https://yourhealthyprostate.com/natural-treatment-of-enlarged-prostate-and-prostatitis/
Best regards
Max.
Hello Max,
Thank you for your response. I was wondering if the decoction was still effective without the use of enemas, and if enemas are mandatory, are there any alternatives to enemas that I may use such as a suppository or such. Also, what is the most effective treatments and lifestyle changes do you recommend for the cure of prostatitis. For reference, I am a 21 year old male, 140lbs, never been sexually active who is diagnosed with chronic prostatitis. My symptoms are testicular pain (primarily following ejaculation), erectile dysfunction, and urinary incontinence for upwards of 2 years. I am hopeful that my treatment and cure lies in Eastern medicine rather than the numerous antibiotics I have been fed the last few months. A detailed treatment would be highly recommended, as I am getting desperate and the pain intolerable. Thank you so much for your time and consideration.
Hi Gabriel
If you are looking for alternatives to enema you can find some suppositories on eBay. I’d recommend S. with shilajit and propolis to start with. They are well known for their anti-inflammatory and antibacterial properties.
Lifestyle hints to prevent or ease prostatitis symptoms you can find here:
https://yourhealthyprostate.com/natural-treatment-of-enlarged-prostate-and-prostatitis/
https://yourhealthyprostate.com/lifestyle-to-mitigate-prostatitis-symptoms/
And I’d strongly recommend giving up junk food, drinking at least 8 cups of water a day to lower inflammatory processes in the body.
Stretching exercises for the pelvic area are recommended in many modern clinics and you can find some of them here:
https://yourhealthyprostate.com/cure-prostatitis-and-chronic-pelvic-pain-syndrome-by-chinese-medicine-practices/
Hope you’ll find the tips helpful.
I’d appreciate it if you keep me posted about your healing progress.
Have a great day!
Max.
Hello Makhsud
Thank you for sharing your journey and thoroughly detailed information.
I tried to research but could not find the reason online, I quote “As to my suggestions in my blog, at least they worked for me. As I noted in the blog I excluded Willow Herb from my recipe, because of its strong hormonal effect.”
What effect, obviously undesirable does it have please?
Looking forward to trying your method and praying for success ?
Many Thanks
….Andreas
Hi Andreas
Thank you for stopping by my blog and asking a question.
“I excluded Willow Herb from my recipe, because of its strong hormonal effect.” First of all, I want to point out that the results of such experiments are rarely predictable. Initially, I tested the composition of the decoction without Willow Herb and noticed a significant improvement in my condition. Later I added Willow Herb, but I used a full tablespoon of it just like Eucalyptus leaves. At first, I was delighted with the result, but soon I discovered what I called the “strong hormonal effect”. I could not sleep normally because of an abnormal erection, which came as soon as I fell asleep. It happened every night and lasted for hours, because of which I had to get up to calm down. Perhaps this has nothing to do with hormones, but how to explain such an effect is difficult for me. Fortunately, after about a month after I stopped all enemas, everything returned to normal. Therefore, I recommend adding only half a teaspoon of Willow Herb or eliminating it altogether. You can use your own herbs or other anti-inflammatories; with enemas, unlike teas, you will get a quick response and result.
Hope it will help to ease your condition!
Hi Max
Thanks for clearing that up for me, question the shilajit ,did you use resin or powder form, you mention 150-200mg they sell it in 10 g jars from what I have seen, so 150mg is equal to 0.15 g is that correct?
I cannot do anymore antibiotics it is destroying my stomach flora..
Tell me have you heard of the Rezum therapy for enlarged prostate… my friend in OZ has had success with it.
How does one confirm which type of prostatitis one has or if it is even prostatitis or maybe just bph?
Sadly so little accurate data on the net.
Are you now completely healed or are you having to maintain the procedure periodically.
Apologies for all the questions, but my quality of life is severely impacted by this condition, and I am so hoping to be able to alleviate my discomfort.
Thanks in advance
Best Wishes
Andreas
Hi Andreas
Sorry for the late reply, I’m on the vacation now.
Your calculations are correct.
In the past, I used resin shilajit, they provide a small spoon to make it easy to grab how much you need. But lately, I ordered shilajit in drops, it seems, 150 mg of the resin in a drop, I’m using 2 drops for an enema.
Tell me have you heard of the Rezum therapy for enlarged prostate.
Rezum therapy or Water vapor thermal therapy has been approved by the FDA in 2015. WVTT and Prostatic urethral lift are the only alternatives to Transurethral resection recommended by the American Urological Association for those who want to have their sexual function unaffected. I would say, currently, WVTT is the most effective minimally invasive surgical procedure that gives good results in easing BPH symptoms with fewer side effects.
You can read more about the effectiveness, pros, and cons, and comparisons of the most popular BPH treatment ways here:https://yourhealthyprostate.com/benign-prostatic-hyperplasia-comparison-of-different-ways-of-treatment/.
Are you now completely healed or are you having to maintain the procedure periodically?
I use the described enemas from time to time, once every two to three months for prophylactic purposes. As for the night trips to the restroom, they hardly bother me, no more than once a night.
Best regards
Max.
Hi Max,
Thank you for your website and all shared info through it. Could you please comment on claims that Shilajit contains some metals like Lead? Also could you please share how often you need to use enemas ones you get rid of the symptoms?
Hi Denys,
The company “Pure Himalayan Shilajit”, where I usually order shilajit and which I recommend to my readers, claims: “Our shilajit is top quality with regard to heavy metal safety standards” and provides the report of a third party US-based laboratory testing for heavy metals.
I personally practice one enema in about two months as a preventive measure, but this can be individual for each person, depending on his lifestyle, occupation, and frequency of contact with risk factors.
Best regards
Max.
Hi Makhsud,
I was diagnosed with chronic bacterial prostatitis at the beginning of the year. Since then, I have had two unsuccessful courses of antibiotics to treat two different types of antibiotic-sensitive bacteria to treat both the prostatitis and recurrent UTI’s.
What is your take on claims that phage therapy may be one of the best ways to treat chronic and recurrent UTI’s associated with chronic bacterial prostatitis since phace therapy offers the advantage of being able to penetrate, attack and clear bacterial biofilms.
Kind regards
Jordi
Hi Jordi
In my opinion, phage therapy looks promising theoretically, but unfortunately, there are no clinically proven results showing that it works superior to traditional antibiotic treatment.
Some of the papers published lately on phage therapy:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6034095/
https://pubmed.ncbi.nlm.nih.gov/32949500/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8222915/
Most of the research on phage therapy has been done in Eastern countries. The results of the only randomized, placebo-controlled clinical trial published in 2021 in the PubMed journal showed that “Intravesical bacteriophage therapy was non-inferior to standard-of-care antibiotic treatment, but was not superior to placebo bladder irrigation, in terms of efficacy or safety in treating UTIs in patients undergoing TURP.”
And you can find a case report of the successful application of phage therapy to treat bacterial prostatitis. Pranav J. first published his cure in his blog three years ago, and in 2021, they described this case in the PMC journal. I know miracles happen, but it would be much more convincing if there were more success reports.
Anyway, it’s only my personal opinion. Do your deeper careful research. I’d appreciate it if you kept me informed about your progress.
I wish you a happy coming Christmas and New Year holidays!
Best regards
Makhsud.
Hi Max
Thanks for clearing that up for me, question the shilajit ,did you use resin or powder form, you mention 150-200mg they sell it in 10 g jars from what I have seen, so 150mg is equal to 0.15 g is that correct? Please! Reply to this
Hi,
Yes, your calculations are correct. Btw, they also sell shilajit in dry drops, 120 drops on a plate, 200mg each. That’s what I bought the last time; it makes it much easier to get what you need.
Prostate cancer screening and early detection do NOT save men’s lives. Let’s do the math. Per the USPSTF (U.S. Preventive Services Task Force): “Only one man in 1,000 could possibly have a life-saving benefit from screening” and “A small benefit and known harms from prostate cancer screening.” However, 1.3 to 3.5 deaths per 1,000 and up to 6.9% hospitalization from a prostate blind biopsy infection or complication. Also, 5 men in 1000 died, and 20.4% had one or more complications within 30 days of a prostatectomy. This does not include deaths, injuries, and side effects from radiation and other procedures, medical mistakes, 5 times higher suicide risk, ADT therapy complications, heart attracts, depression, low quality of life, etc., caused by prostate cancer screening and treatments. Detection and overtreatment of prostate cancer has killed or destroyed millions of men’s lives worldwide from understated and multiple undisclosed side effects. The doctor that invented the PSA test, Dr. Richard Ablin now calls it: “The Great Prostate Mistake,” “Hoax”, “Misused”, “Unreliable” and “A Profit Driven Public Health Disaster”. Follow the money!
https://www.youtube.com/watch?v=tYii98gcejA
https://medium.com/@drsadeghi/early-detection-disaster-4d4740ee5828
https://urologyweb.com/uro-health-blog/
https://grossovertreatment.com
https://medium.com/@bvorstman/is-psa-testing-for-prostate-cancer-bad-health-advice-7199618e56c5
https://www.youtube.com/watch?v=0IHE9jdCpn4
https://www.sciencedaily.com/releases/2018/03/180306141708.htm
Recommended books:
The Great Prostate Hoax by Richard Ablin MD (the inventor of the PSA test)
The Big Scare, The Business of Prostate Cancer by Anthony Horan MD.