Last Updated on July 7, 2024 by Max
Introduction
Here, I will guide you step by step on how I envision the causal relationship between the events taking place in our body and resulting in prostate cancer. At the end of the post, you will have a holistic picture of how prostate cancer arises and the importance of diet and a healthy lifestyle in preventing prostate cancer.
- Introduction
- The Causal Relationship of Prostate Cancer Arising
- Basic Knowledge About Prostate and Prostate Cancer
- The Structure of the Prostate: Prostate Cancer Arising Sites
- Evidence-Based Studies Show a Link Between Colorectal Health and Prostate Cancer
- How Is Your Prostate Connected to Your Rectum?
- How Does Your Diet Increase the Risk of Prostate Cancer?
- How Does Constipation Affect Your Prostate Health?
- Conclusion
- Literature
The Causal Relationship of Prostate Cancer Arising
- Like any other type of cancer, prostate cancer starts when the prostate gland cells mutate into cancer cells and begin to grow out of control.
- No natural food humanity has been consuming for millions of years of its evolution is capable of causing genetic or epigenetic alterations in the structure or function of the genes. If there are some, they must be negligible; otherwise, we’d have avoided this food.
- Only carcinogens, mostly chemically synthesized like pesticides and herbicides, or naturally occurring in our body under unusual conditions like hydrogen sulfide and N-nitroso-compounds, or local imbalance of steroid hormones in the prostate are capable of triggering cell malignancy.
- The main route to how these carcinogens get inside of your body is your digestive system.
- The colon and rectum, as the last parts of the gastrointestinal tract, accumulate all the solid and liquid wastes, including genotoxins, and separate the liquid from the feces filtering the former back into the blood.
- The prostate is located in the vicinity of the rectum and has a shared arterial vasculature, so there is a good chance for all kinds of carcinogenic substances to get directly into the prostate and trigger cancer growth.
- An unbalanced diet, some medicines, antibiotics, and constipation may cause the balance of healthy gut microbiota to change; sulfate- or nitrate-reducing bacteria multiply, producing more and more carcinogenic toxins. When the concentration of toxins in your bowel is too high, they begin to leak outside, leading to prostatitis or prostate cancer.
- Some toxins, while not carcinogenic, may cause epigenetic changes and activate some genes, including aromatase, which in turn increases estrogen levels in the prostate. Estrogens are steroid anabolics with mild mutagenicity and may trigger carcinogenicity in couples with testosterone and support prostate cancer growth.
Let’s analyze the available scientific data and combine two and two.
Basic Knowledge About Prostate and Prostate Cancer
The prostate is a walnut-sized exocrine gland of males, contacting the bladder carrying liquid wastes from one side and the colorectum carrying fecal wastes from another side. This unfavorable proximity of the prostate to the potential sources of irritants and genotoxins plus prostate enlargement caused by varicocele determine its fragility and vulnerability.
Statistics say that there has been a 60% increase in prostate cancer incidences in American men since 1975. American Cancer Society predicts that one man in 8 will be diagnosed with prostate cancer. Fortunately, most men diagnosed with prostate cancer survive, which is not the main reason they die.
However, according to the findings published in the Journal of Prostate Cancer and Prostatic Diseases, the number of metastatic prostate cancer in 2013 was from 72 to 92 percent higher than that in 2004. Metastatic prostate cancer is the most aggressive cancer and is not curative. They also found that the average prostate-specific antigen of men with metastatic prostate cancer in 2013 was 49, whereas, in 2004, it was only 25, which hints that more aggressive disease is on the rise.
Most prostate cancers are adenocarcinomas; they originate from the mutation in the semen-producing prostate gland cells. Some prostate cancers can expand fast, but most grow slowly. Studies of males who died from irrelative causes have found prostate cancer in 30% to 70% of those over age 60. In many cases, neither they nor their doctors even knew they had it.
The Structure of the Prostate: Prostate Cancer Arising Sites
At the functional level prostate gland consists of the glandular part (~66%) responsible for its secretory capacity and a fibromuscular portion (~33%) helping semen discharge during ejaculation.
Structurally prostate can be divided into four zones:
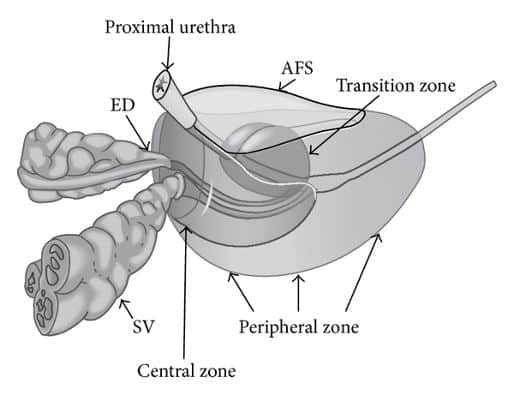
So, is it only by chance that 80% of prostate cancer cases are found in the PERIPHERAL ZONE, the closest site to the RECTUM? Let’s examine if there is any connection between prostate cancer with colorectal conditions.
Evidence-Based Studies Show a Link Between Colorectal Health and Prostate Cancer
In 2010 researchers at the Buffalo University first reported that men with prostate cancer are at increased risk of developing colon cancer. They analyzed the colonoscopy results of 188 patients diagnosed with prostate cancer and compared them with the control patients. Prostate cancer patients had 48% adenomas and 15.4% advanced adenomas, whereas in control – only 30.8% and 10%, respectively.
One more study in 2003 investigated the relationship between colorectal and prostate cancer. They found that men who develop colorectal cancer risk two times more prostate cancer.
As a reported study from Northwestern Medicine, the risk of being diagnosed with prostate cancer is four to five times higher for men with inflammatory bowel disease (IBD). In this study, 1,033 men with IBD and a control group of 9,306 men without the disease were followed up for 18 years.
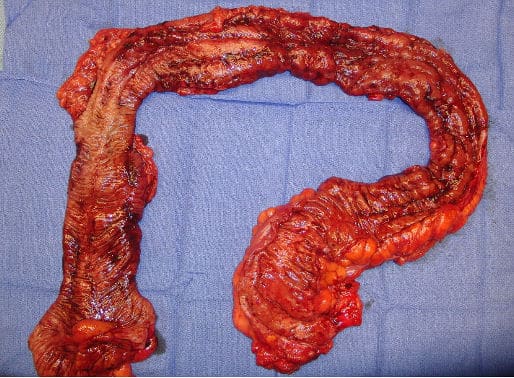
Inflammatory bowel disease (IBD) is a group of inflammatory conditions of the colon and small intestine. Crohn’s disease and ulcerative colitis are the principal types of inflammatory bowel disease. Crohn’s disease affects the small intestine and large intestine, as well as the mouth, esophagus, stomach and the anus, whereas ulcerative colitis primarily affects the colon and the rectum.
https://en.wikipedia.org/wiki/Inflammatory_bowel_disease
Do not all this evidence-based data demonstrate that your bowel and prostate are connected and affect each other? They are not only related but also operate as two communicating vessels.
Let’s check how they are connected.
How Is Your Prostate Connected to Your Rectum?
- Prostate gland vasculature mainly comes from the prostatic arteries, but some branches may also arise from the internal pudendal and MIDDLE RECTAL ARTERY. The middle rectal artery is distributed to the rectum and is in charge of its arterial blood supply. So if the prostate and the rectum have a common vasculature, at least partially, I would strongly suggest they exchange all chemicals getting inside of the bloodstream too.
- As I mentioned earlier prostate gland is located in the vicinity of the rectum, and with age, the prostate may enlarge several times in size, even pressing into the wall of the rectum. When your bowel is working correctly, the feces are eliminated in time, and the level of exogenous and endogenous toxins in the feces is low, the wall of the rectum performs its barrier function perfectly; even if the content of the bowel has a high level of toxins, their exposure time to the wall of the colon is short. But if your food contains one too many toxins your bowel is out of order, and you have an altered microbiota producing endotoxins, I would strongly expect a leakage of toxins through the rectum wall into the surrounding space. It is a common phenomenon when a certain organ has been affected, it makes visible changes in the surrounding organs; it can be detected upon autopsy easily.
So now we know that eating or drinking something toxic will affect your prostate, but if the toxins are carcinogens, they may cause tumor growth in your prostate.
How Does Your Diet Increase the Risk of Prostate Cancer?
I hold the point of view that any food is beneficial to your health if it is consumed in moderation. Of course, if your metabolism is not working correctly and you have a disease in your body, it is advisable to stick to a special diet and avoid some specific foods.
The previous post analyzed how and why meat can cause prostate cancer. I am rehashing here; it is not about meat only; any food, if it is loaded with pesticides, fertilizers, hormones, or any other chemical with genotoxic effect, may cause prostate cancer.
As I mentioned earlier, even if we consume pesticide-free, fresh food cooked in the most gentle way, we still have a chance to increase the odds of prostate cancer due to the abnormal metabolism of our gut flora. Here, I’ll repeat the fragment of the previous post about how your gut microbiota may increase the risk of prostate cancer.
There is not much evidence of a relationship between gut bacteria metabolism and prostate cancer in the literature. However, multiple studies suggest gut flora affects the incidence of colorectal cancer and that there is a linear association between prostate cancer and colorectal cancers.
Bacteria live in the gut system of any animal species, from insects to humans. If only a few bacteria species have been found in the stomach and small intestine, the colon is densely populated with more than 500 different species. Bacteria make up to 60% of the dry mass of feces.
Sulfate Reduction. Sulfate-reducing bacteria (SRB), as a part of the normal gut flora, contribute to the immune response stimulation in the gut, but when their number increases enormously, they may contribute to colitis development mediated by hydrogen sulfide (H2S) production. Hydrogen sulfide is a hazardous gas with a “rotten egg” smell. It can be produced by the decay of human and animal organic wastes. Hydrogen sulfide has the potential to damage genomic DNA, causing genotoxic effects in the gut cells. Meat proteins are rich in sulfur-containing amino acids, and a meat diet may result in SRB abundance and therefore contribute to H2S formation, increasing the risk of colorectal cancers.
Nitrate reduction. Some species of bacteria in the gut can reduce nitrates to nitrites via nitrate reductase. The subsequent interaction of nitrites with organic substances results in the production of NOCs-carcinogens mentioned earlier. Red and processed meat, rich in protein and other nitrogenous residues, may support increased production of NOCs by gut bacteria. The more you eat meat, the more nitrogenous residues get into your colon. Nitrosamines, nitrosamides, and nitrosoguanidine are classes of NOCs found in feces. NOCs can form DNA adducts- segments of DNA bound to a cancer-causing chemical, which induce mutations.
Unlike red and processed meat, which contain heme iron in abundance, and produce increased fecal NOCs, white meat and vegetable protein did not increase fecal NOCs. Heme iron is an essential part of hemoglobin, the red pigment in blood, and myoglobin, the principal oxygen-carrying pigment of muscles. Higher levels of myoglobin in muscles allow diving animals such as whales to hold their breath for a more extended period. So, heme iron, a specific part of red meat, can catalyze NOCs formation and may be responsible for the additional dose-dependent N-nitrosation in the gut. The addition of soy may significantly suppress fecal NOCs.
It looks like gut microbiota represents a cocked trigger ready to work at any moment. The triggering factors may be diet, medicine, especially antibiotics taken inside, or constipation.
Here we’ve got to the point of how constipation may affect prostate health.
How Does Constipation Affect Your Prostate Health?
Most of the end absorption of the food nutrients (about 90%) takes place in the small intestine. The remaining waste products containing toxins move further into the digestive system and accumulate in the large intestine or colon, where absorption of water takes place and should be eliminated then.
But if you are constipated, the remaining organic matter begins to rot. The balance of healthy gut microbiota changes, and sulfate- or nitrate-reducing bacteria multiply, producing more and more carcinogenic toxins. When the concentration of toxins in your bowel is too high, they begin to leak outside, affecting the adjacent organs and the prostate particularly. A buildup of toxins in the prostate leads to its poisoning, inflammation takes place, the prostate gets painful, and eventually, you may have all the typical symptoms of prostatitis. Likewise, the toxins may cause prostate cancer.
It is evident that the role of constipation in triggering prostatitis and prostate cancer is underestimated.
More information about constipation and its effect on the prostate can be found in the post “How constipation affects your prostate?“
Conclusion
The post is written for those caring to have a healthy prostate.
The human body is the pinnacle of nature’s creativity, where tens of thousands of genes operate in harmony. When some toxins change the correct work of the genes, it’s the same as if some dirt gets inside of the perfectly tuned watches. The only way to fix the watches – clean them from the dirt. When we are trying to design drugs to correct the function of the genes, it is the same as if one tries to wash off one dirt with another dirt.
Based on the preceding, I would strongly suggest the following recommendations to lower the risk of prostate cancer:
- Diversify your diet; both animal and vegetable food should be included in your diet.
- Eat healthy food without pesticides, synthetic fertilizers, and hormones. At least try to gradually replace the most popular products on your table with organic ones.
- Eliminate or reduce the amount of processed food in your diet.
- Take care of your gut health; change your lifestyle to avoid constipation.
- Keep your hormonal balance under control.
It’s up to you which way to choose: the way of preventing or the way of treating prostate cancer.
Literature
- Anil Bhavsar and Sadhna Verma. Anatomic Imaging of the Prostate. BioMed Research International. Volume 2014.
- University at Buffalo. “Prostate cancer patients are at increased risk of precancerous colon polyps.” ScienceDaily. ScienceDaily, 19 October 2010.
- Moot AR et al. Men with colorectal cancer are predisposed to prostate cancer. ANZ J Surg. 2003 May;73(5):289-93.
- Jacob A. B. et al. Inflammatory Bowel Disease and the Risk of Prostate Cancer. European Urology, 2018; DOI: 10.1016/j.eururo.2018.11.039


In my opinion, in order to avoid prostate cancer, natural food is the necessary divine food, the connection with nature and movement, sports, walks of at least an hour a day are necessary for a healthy body, and the use of natural remedies like teas, who are all of God for us, but we forgot to go back to the ancestral wisdom and take everything from nature.
How is early detection done?
There are many ways: tumor markers such as PSA blood tests, visits to the doctor if there is any family can make even imaging investigations. In the past two years, there has been a real revolution in the diagnosis of prostate cancer with the help of multiparametric prostate MRI, which was not available before. The way prostate cancer is being developed has developed a lot: we can do this earlier and more precisely, and because of this we can treat it more effectively. The link between the colon and the prostate, in fact, the connection between colon and prostate cancer is inherently linked to toxins that cannot escape from the body due to constipation but also to food products filled with chemical products found in different foods and which the body transforms them from healthy cells into cancer cells that are rapidly growing. In my country, in Romania, there are 4,500 patients with this disease every year.
Dear Alina
Thank YOU so much for honoring me with your time by reading my post and commenting! Yes, you are right, we are losing the connection with NATURE, but as the Nature creatures, we cannot live outside it. This increasing disbalance reflects in man as a rocketing rise of body and mental disorders. The earlier we understand it, the less painful will be the way back.
Development of accurate diagnostic tools for prostate cancer definitely allowed to save millions of lives lately. But, unfortunately, the relative number of men affected with prostate cancer still is progressing. My understanding is that this process can be slowed down or stopped only if we change our lifestyle, and our attitude to the food we nourish our body.
Wishing you allthe best
Makhsud
This post comes at an opportune time for me as I am very open and educational to my son about his anatomy and the function of his body. I do this so that he has an awareness of himself, his system and so that in his formative years I can download to his belief system the value and empowerment that comes in understanding your body’s system and how to care for it in an optimal manner. He asked me only yesterday about the baby making process and I spoke to him about ejaculation and the seed etc but I didn’t know how the ejaculatory system worked and was at a loss as to how to explain it to him when he asked “how does it squirt out?” Never did I think that I would be a woman enraptured by this post on a prostate but here I am presently feeling very grateful and most enlightened by the mechanism that is the prostate and my new knowledge of it and fibromuscular tissue of the anterior zone contraction.
It is very interesting to me too, the close proximity of the prostate to sources of irritants and wondered if that was a fundamental design and nature’s way of ensuring a man take care of his physical health optimally and make more natural choices aligned with the earth given its vulnerability. It is a curious thing to me that the practice of chemicals, hormones and pesticides are even allowed to be in the vicinity of consumables, let alone in the production of consumables. When did humanity become so reckless with our care and lose such esteem in our worth to normalize and enable such a practice? Your facts regarding natural foods being unable to cause genetic or epigenetic alterations in the genetic structure/function of a persons genes supports my ideals that we should be nourishing and enhancing the natural world and ourselves in a simple, natural and balanced way and living abundantly from it, rather than depleting it and contaminating ourselves with chemically laden entities.
Your post is very insightful and informative. I believe that knowledge is power and when a man takes self responsibility and understands the impact his choices has on his gut health and ultimately his prostate, then it can yield a very empowering and healthy lifestyle.
Great insights and very useful information on many fronts!
Thank you Makhsud!
Thank you so much, Rebecca, for your comment. It is always pleasant to know that your efforts were not in vain, and when you get such kind of comment, it encourages you to the new investigations. I’m sure that we have to discuss with our children not only the functions and structure of our body but the causative relations of body disorders and illnesses as well. That way they will escape an unhealthy lifestyle, habits and will know better than any doctor what is the cause if something happens with their health. The more I’m communicating with people the more I’m getting convinced that ignorance especially as to reproduction organs and their functions and hygienic is widespread not only among the low educated category of our society but in academic circles as well.
Yes, I’m for the natural food; all functions of our enzymes and cell and body metabolism evolved during millions of years to use some foods and avoid the others. For just only last hundred years we have contaminated our food so much that there is no wonder why we have a skyrocketing of diseases.
Hope you found some useful information in the post and thank you again for stopping by my site and commenting.