Last Updated on July 7, 2024 by Max
Introduction
Testosterone is pivotal for maintaining efficient metabolic processes throughout the body. However, as men age, testosterone levels naturally decline, leading to reduced bioavailable testosterone and its associated benefits. According to the Baltimore Longitudinal Study of Aging, rates of hypogonadism (characterized by reduced testicular size) are reported as 20% in men over 60, 30% in men over 70, and 50% in men over 80.
Testosterone Replacement Therapy (TRT) can significantly enhance the quality of life for men with low testosterone levels. Still, it’s crucial for anyone considering TRT to fully comprehend the potential risks involved. TRT is contraindicated for men diagnosed with prostate and breast cancer. Those undergoing TRT should vigilantly monitor for potential side effects such as polycythemia, edema, and cardiac and hepatic dysfunction (Osterberg EC et al., 2014).
Potential Health Risks of TRT and Key Monitoring Strategies
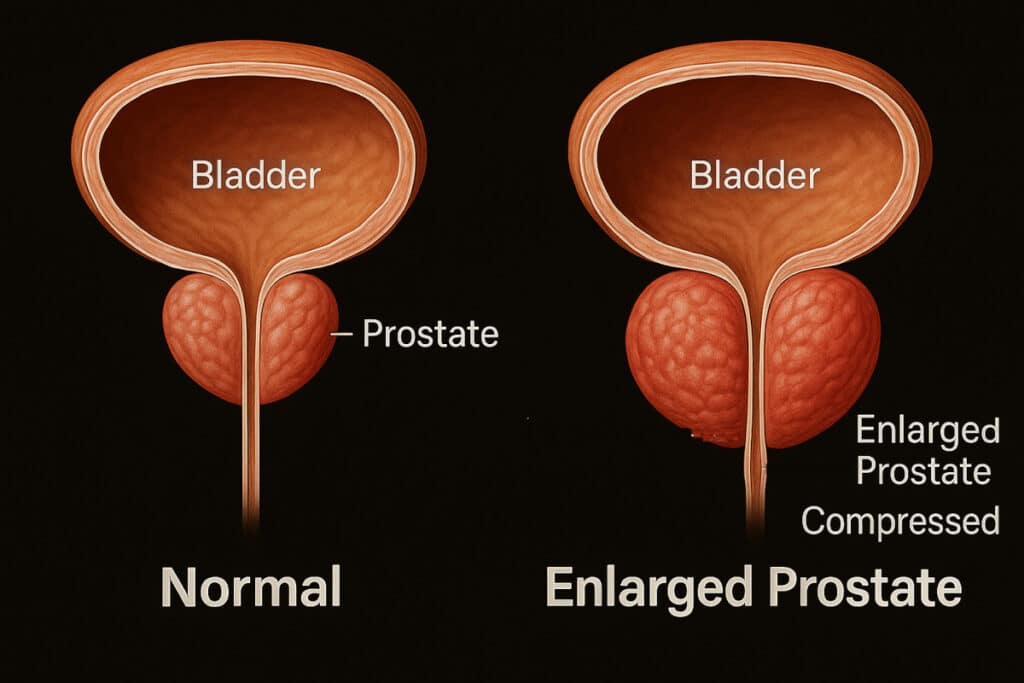
Patients with health conditions that exclude the possibility of TRT should be thoroughly informed about all associated risks. When prescribing TRT, healthcare providers should consider the potential for exacerbating prostate cancer, worsening benign prostatic hyperplasia symptoms, increasing the risk of male breast cancer, polycythemia, obstructive sleep apnea, and the heightened risk of arterial plaque buildup.
Potential risks of TRT and associated monitoring strategies (From Osterberg EC et al. 2014)
| Potential Risk | Suggested monitoring strategies |
| Cardiovascular disease | Baseline blood pressure checks and repeated at 3 and 6 months, then annually thereafter. For high-risk patients, consider cardiology referral |
| Erythrocytosis | Obtain baseline HCT then at 3 and 6 months, then annually thereafter. If HCT is >54%, stop TRT and restart at a lower dose!*”! |
| Fluid retention | Patient history and physical exam. Stop TRT if CHF is uncontrolled.” |
| BPH | Patient questionnaire and history. Refer to a urologist if: IPSS+above 19 and stop TRT! |
| Prostate cancer | Obtain baseline DRE and serum PSA then again at 3 and 6 months. Continual monitoring depends on the patient’s race/age. Refer to a urologist if: Abnormal DRE; PSA rises over four ng/mL; If PSA rises more than one ng/mL in the first six months; of TRT or by more than 0.4 ng/mL/year thereafter 4; If PSA velocity is more than 0.4 ng/mL/year! |
| Acne | Patient history and physical exam. Dose adjustment and/or referral to dermatology |
| Hepatoxicity | Patient history and physical exam. Liver function tests are unnecessary in gel, pellet, and IM preparations |
| Infertility | Patient history and physical exam. Reconsider alternative strategies if the patient desires to father children |
| OSA | Baseline patient history and physical exam and again between 3 and 6 months.! Consider alternate causes of OSA! |
| Gynecomastia/ breast cancer | Exclude other etiologies with patient history and physical exam. Review all medications. Complete hormone evaluation may be necessary. Medications implicated in causing gynecomastia! Anti-androgens-finasteride, bicalutamide Antibiotics-isoniazid, ketoconazole, metronidazole Antihypertensives-amlodipine, captopril, diltiazem, verapamil, nifedipine Gl agents-cimetidine, omeprazole Psychiatric-diazepam, haloperidol, tricyclic antidepressants |
CHF=Congestive heart failure, IPSS=International prostate symptom score, PSA=Prostate-specific antigen, IM=Intramuscular,
OSA=Obstructive sleep apnea, Gl=Gastrointestinal.
A Closer Look at Endogenous vs. Exogenous Testosterone
Often, medical professionals emphasize the benefits of TRT using scientific evidence regarding the effects of endogenous (naturally occurring) testosterone on health, inadvertently neglecting to discuss potential adverse side effects associated with exogenous (externally administered) testosterone therapy. It’s important to note that these two forms of testosterone can sometimes have divergent effects, the reasons for which are not fully elucidated.
Let’s consider the cardiovascular impact of endogenous and exogenous testosterone. Here’s a segment from a post advocating TRT:
“A study focused on the correlation between blood testosterone levels and cardiovascular events, such as heart attacks and strokes. The study involved 2,416 men aged 69-81, not on any testosterone-affecting treatment. It was observed that men with increasing testosterone levels had a decreased prevalence of diabetes, hypertension, and body fat mass. Men with the highest testosterone levels were the most physically active and demonstrated a 30% lower risk of cardiovascular events when testosterone levels exceeded 550 ng/dL. The study concluded that higher serum testosterone levels are associated with a reduced risk of fatal and non-fatal cardiovascular events in elderly men” (Ohlsson C et al. 2011).
While these findings underscore the benefits of endogenous testosterone, the same cannot be said confidently about exogenous testosterone administered through TRT. Several research studies, including a recent report by Peter J. Snyder and colleagues (2018), indicate a positive correlation between TRT and cardiovascular events.
The Cardiovascular Trial, part of the Testosterone Trials (TTrials), involved 788 men with a mean age of 72. It was discovered that testosterone treatment significantly increased the volume of noncalcified plaque in the coronary artery, which is directly related to the risk of fatal cardiovascular events. Furthermore, polycythemia, a condition marked by an elevated volume of red blood cells, is a recognized side effect of TRT. This condition can thicken the blood, slow its flow, and potentially cause severe cardiovascular problems, such as blood clots.
As you can see, the effects of high testosterone levels in older individuals can vary significantly depending on whether the testosterone is endogenous or exogenous. Consequently, using research results related to natural, endogenous T to promote TRT is at least misleading.
The Appeal and Risks of TRT in Younger Men
While TRT can offer significant benefits, particularly to older men with declining testosterone levels, it also attracts younger populations who may not fully understand the potential risks. For example, young or middle-aged men might be tempted to use TRT rather than opting for lifestyle changes to boost testosterone production naturally. These individuals often do not realize the potential health risks they could be facing.
Consider this example from a social network post: a man who started TRT in 2017 had to undergo angiograms in 2019 and again recently due to over 80% blockage in three main arteries. His doctors attributed the plaque build-up, at least in part, to his TRT use. The individual was active and maintained a healthy diet, yet experienced significant cardiovascular complications, potentially related to TRT.
The Complex Interplay of TRT and Overall Health
When testosterone levels decrease due to age, illness, or lifestyle, a cascade of changes occurs in the body that we might not fully understand. While lifestyle changes, diet, and exercise can naturally boost testosterone levels and bring balance to the body, using TRT can disrupt this harmony.
In the case of TRT, elevated testosterone levels might not fit into the complex relationships of other biologically active components, preventing the full manifestation of health benefits and potentially leading to unexpected adverse effects. This balance disruption is especially significant concerning the cardiovascular system.
The explanation sounds mechanistic, and I couldn’t find scientific data. However, I believe that we must be very careful when we disrupt the balance and hormones of important components such as testosterone to not turn it from an element of youth into a factor of destruction to our body.
Revisiting the Results of the TTrials
The Testosterone Trials (TTrials) was a comprehensive study investigating the effectiveness of increasing testosterone levels in older men with low testosterone. This study included various trials, such as Sexual Function, Physical Function, Vitality, Cognitive Function, Anemia, Bone, and Cardiovascular diseases.
The trials found that testosterone treatment led to a substantial increase in sexual activity, a slight improvement in walking distance, and improved mood and depressive symptoms, albeit without increasing energy. There was no observed improvement in cognitive function, but testosterone increased hemoglobin levels and improved bone mineral density.
However, testosterone treatment also increases noncalcified plaque volume in the coronary artery, raising the risk of fatal cardiovascular events. While the trial did not associate testosterone with more cardiovascular or prostate adverse events than a placebo, the authors concluded that a longer trial would be necessary to determine whether testosterone increases cardiovascular or prostate risk.
Conclusions
Human health has long been a significant concern, with increased chronic diseases, including cancer, cardiovascular, and autoimmune diseases. As such, the number of clinics focused on correcting hormonal balance, particularly through TRT, has risen rapidly.
Before deciding to embark on TRT, being aware of all associated risks is crucial. Regular monitoring for potential adverse side effects is essential if you’ve chosen TRT to enhance the quality of your life. As with any medical intervention, a thorough discussion with healthcare professionals is crucial to make an informed decision that balances benefits and risks. Consider natural alternatives, like exercise and diet modification, before resorting to hormonal replacement therapies.
TRT can be a powerful tool for improving the quality of life for men with low testosterone levels, but it’s not without potential complications. More comprehensive and long-term studies are needed to fully understand the benefits and risks of TRT, especially concerning cardiovascular health and prostate cancer. Until then, caution and close medical supervision are paramount for those considering or undergoing TRT.
Literature.
- Osterberg EC, Bernie AM, Ramasamy R. Risks of testosterone replacement therapy in men. Indian J Urol. 2014;30(1):2-7. doi:10.4103/0970-1591.124197.
- Ohlsson C, et al. High serum testosterone is associated with reduced risk of cardiovascular events in elderly men. The MrOS (Osteoporotic Fractures in Men) study in Sweden. J Am Coll Cardiol. 2011 Oct 11;58(16):1674-81. doi: 10.1016/j.jacc.2011.07.019. PMID: 21982312.
- Snyder PJ, Bhasin S, Cunningham GR, et al. Lessons From the Testosterone Trials. Endocr Rev. 2018;39(3):369-386. doi:10.1210/er.2017-00234.